Balls and Walnuts
more than you ever wanted to know
- About
- All Change
- Big pix
- Dormies
- Ear, Nose, Throat, and Soul
- Heaven on Earth
- Karen’s memoriam . . . booklet and eulogy
- Lyvvie’s email
- Magic Schoolbus does your nose and throat
- Nest: scene one
- Sex and the Single Wendigo
- Sprouts
- The Mechanic
- Two Birds, One Stone
- Excerpt: Gator and Shark Save the World
Radiofrequency uvulopalatoplasty for snoring
Yeah, you read that title right. Sometimes I feel motivated to make a public service announcement. Not often, but sometimes, and tonight’s the night. And since the chances are pretty good you (or your spouse) snores, I figure I won’t lose too many of you with a relatively serious post.
This first bit is for my malpractice insurance carrier:
I am NOT offering medical advice; I am merely providing information. Read the disclaimer. It has flashy things and animated buttons to keep you entertained.
Another note: my victim patient, Jeannie, has given me permission to use her images in these blog posts. Wasn’t that nice?

Look, she’s even smiling about it.
Follow me below the fold for a discussion of snoring, obstructive sleep apnea, and the use of radiofrequency uvulopalatoplasty to successfully treat snoring.
While many people with obstructive sleep apnea snore, not everyone who snores has obstructive sleep apnea (OSA). What difference does it make? Pretty big one, actually. OSA can kill you (more on that in a moment), snoring can’t (unless your bed partner decides to become fodder for the next season of Law & Order). We treat OSA differently than uncomplicated snoring, so it’s important to learn right from the start which diagnosis the patient has.
Insurance companies wish docs could differentiate between these two diagnoses based on the history, physical exam, bed partner interview, or some simple radiologic procedure. They would like that very much because those “tests” are cheap, while the gold standard diagnostic procedure is expensive. But, unfortunately for the insurance companies, as well as folks who are under-insured or uninsured, the gold standard — a sleep study — is the only way to nail the diagnosis.
We don’t like missing the diagnosis of OSA because of its health consequences. You’ll learn from the linked article that OSA increases the risk of car accidents, depression, high blood pressure, heart disease, stroke, and death. Left untreated, OSA of sufficient severity decreases your life expectancy.
But let’s say you’ve had your sleep study and you don’t have OSA. You snore. That’s it. And that’s enough. What do you do now?
The sprays you can buy in the drugstore and pills you can buy online don’t work. If my son weren’t angling for this computer right now, I’d take the time to dig up the reference, but trust me — some ENTs took a close look at these over the counter “cures” a few years ago and found them inefficacious. That leaves us with the two most common surgical treatments: LAUP (laser-assisted uvulopalatoplasty) and RAUP (radiofrequency-assisted uvulopalatoplasty).
They work by the same method. The idea is to injure the muscle of the soft palate, thus scarring the muscle. This shortens and stiffens the soft palate. Either method can be used to shrink an enlarged uvula, too. The two methods differ in the type of energy used: laser versus electrical current. Yes, “radiofrequency” is a polite, nonthreatening way of saying “electrocution”. Sneaky bastards, aren’t we?
The two methods have one other big distinction: pain. In order to injure the muscle of the soft palate, the laser has to burn its way through mucosa. With RAUP, we use an insulated needle electrode to bypass the mucosa and go directly to the muscle. The mucosa sustains much less injury than with LAUP. Since sensory nerves are more prevalent in the mucosa than in the muscle, LAUP hurts. In fact, depending upon whom you talk to, the pain is legendary. LAUP? Not so much. Most of my patients use ibuprofen, or if they use any narcotic at all, they’re off it within two or three days.
Which brings us back to Jeannie. Say “AH”:
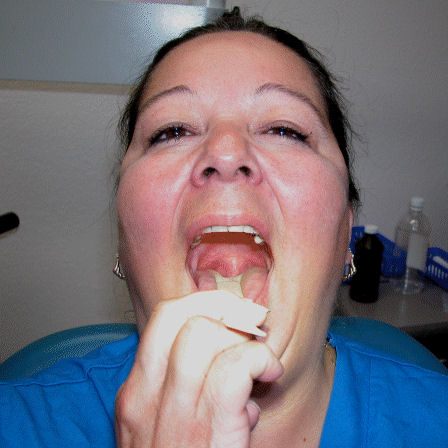
Notice that you can’t see Jeannie’s uvula. Her soft palate is excessively long, so long that her uvula is hidden by her tongue. Even when she presses down with a tongue depressor, her uvula is still playing shy. Compare that photo to this diagram.

In a RAUP, I zap the uvula and soft palate in six or seven different locations. First, however, I inject local anesthetic into the soft palate. This is the least pleasant part of the whole affair, but honestly, it’s not much worse than dental work requiring local anesthesia. Once the soft palate is numb, we begin.

The electrode administers a low current to the tissue. Again, it’s only the tip which is uninsulated. The portion of the electrode in contact with mucosa is insulated. The muscle takes the hit, not the mucosa, which is just the way we like it.
Jeannie will return in four weeks for another treatment. In my experience, it takes three or sometimes four treatments (and sometimes more than that) to create a happy bed partner. That’s the endpoint of treatment, by the way — not “no snoring,” which is difficult and unrealistic, but “my husband sleeps through the night, now,” which is really all that matters.
Does it work? I’ve been a bad scientist — I haven’t tracked my own results — but my impression is, at least 75% to 80% of my patients are happy customers. I’ve been doing this for nine years, and I’ve had relatively few outright failures. In this study, the success rate was 85%.
Most people complain more about post-op swelling than pain. With successive treatments, swelling becomes less of an issue, pain somewhat more, but it’s still manageable with ibuprofen or a few days of a weak opiate. Complications are few: if the electrode is too close to the mucosa, you can get an ulceration, which is a tiny version of what LAUP does on the grand scale. Theoretically, bleeding, infection, and excessive swelling can occur, but in my experience the complications are limited to swelling and pain.
Well, Jake wants this computer, so I’ll wrap it up. Any questions?
I’ll keep you posted on Jeannie.
D.
Cross-posted at the Boogerz Blog.
5 Comments
Find it
Blogroll
- Beth
- Blue Gal
- Charlene Teglia
- Chris and Dean
- Crystal
- dcr, the one, the only
- Erin O’Brien
- Fanatic Cook
- fiveandfour
- Gabriele
- If I Ran the Zoo
- Indecision 2008!
- jmc
- Kate Rothwell
- Kris Starr
- Lyvvie
- Matt’s recovery blog
- Mike Imlay
- Paperback Writer
- Pat Johanneson
- Raw Dawg Buffalo
- Science Blogs
- Shaina
- Shelbi
- Smart Bitches
- Steve Bunche
- Steven Pirie
- Tam’s blog
- The Amanda Files
Archives
Meta
Categories
Pages
- About
- All Change
- Big pix
- Dormies
- Ear, Nose, Throat, and Soul
- Excerpt: Gator and Shark Save the World
- Heaven on Earth
- Karen’s memoriam . . . booklet and eulogy
- Lyvvie’s email
- Magic Schoolbus does your nose and throat
- Nest: scene one
- Sex and the Single Wendigo
- Sprouts
- The Mechanic
- Two Birds, One Stone
i wish we could convince my dad do to a sleep study. no matter how much we tell him YOU STOP BREATHING IN YOUR SLEEP AND THAT’S NOT GOOD YOU DUMBASS he refuses to go to a doctor or do a sleep study or anything. roar. idiot. and then he wonders why he’s so tired, and can’t remember things.
That sounds a lot kinder than the treatment I read about a few years ago where they used a cauterizing tool to sear the soft palate and cause scar tissue to tighten up slack palates. *shiver* the thought of smelling and tasting burnt flesh after that was icky in the extreme.
She has a lovely smile, does Jeannie.
…why didn’t you wear gloves?
Also, I’m curious if this kind of thing would work for slack bladders.
Shaina: would data convince him, or is he too stubborn even for that?
Lyvvie: you’re describing CAUP (cautery-assisted uvulopalatoplasty) which is every bit as nasty as LAUP. Don’t know about bladders, but I do know that folks have used radiofrequency thermal injuries to toughen the lower esophageal sphincter (as a treatment for GERD). As for the gloves — well, I should have, mostly because of patients’ perceptions about such things. But in reality, no part of me comes into contact with the patient, and vice versa. And the mouth is not a sterile place.
even data won’t convince him. he’s not only a dumbass, he’s a stubborn one.
Oh the wonders of modern medicine.
I do snore.
My wife says I do stop breathing in the middle of the night.
The Sleep Test out at the UBC Hospital Sleep Clinic came back negative, tell this guy not to bother us again.
Edwin